A team led by Rice University bioengineers with support from the National Institute of Biomedical Imaging and Bioengineering (NIBIB) used bone engineered into a shape defined by a 3D-printed mold and grown alongside the ribs of sheep to successfully replace a portion of the animals’ jaw bones. The researchers hope to develop the tissue regeneration procedure for human application, so that craniofacial injuries can be treated with bone tissue grown alongside natural bone instead of extracting bone from other parts of the body for grafting and implantation.
“Restoring bone structure lost through injury or disease is an important goal for tissue engineering research,” said Šeila Selimović, NIBIB program director in Technologies for Tissue Chips, Engineered Tissues, and Physiological Biosensors and Detectors. “The research applies a complex process that makes innovative use of biomaterials and tools such as 3D printing to generate bone tissue for jaw reconstruction.”
The human jaw sustains repetitive force while biting and chewing a varied diet of solid foods. Sheep use similar biomechanics to macerate feed pellets and hay. A set of muscles connected to the bone work in combination, rotating the lower jaw (or mandible) up and down and from side to side. When an injury or illness causes damage to the jaw and tissue loss, bone implants are sometimes required to reconstruct the jaw, which must be able to replicate this hard-working anatomical structure.
A multi-institution team, led by bioengineer Antonios Mikos, Ph.D., Louis Calder Professor of Bioengineering and Chemical and Biomolecular Engineering at Rice University and director of the NIBIB-funded Center for Complex Tissue Engineering, conducted the sheep study based on the team’s vision for a process, called biomaterial-assisted mandibular reconstruction. The team includes members of the University of Texas Health Science Center at Houston.
“We are pleased to contribute a regenerative solution for the potential treatment of craniofacial defects,” Mikos said. “This work is a testament to the value of team science.”
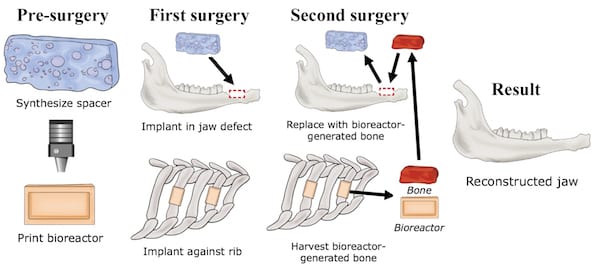
In their study, published in the Proceedings of the National Academy of Sciences on March 18, 2019, the researchers created rectangular defects in the lower jaws of six sheep. They used a spacer, which temporarily preserved the shape of the jaw at the site of the defect, and produced 3D-printed molds, called bioreactors, which are used to grow replacement bone tissue. They filled the bioreactors with biocompatible ceramics or crushed bone, anticipating that each material would be a good medium for growing replacement tissue.
The researchers implanted four bioreactors in each sheep, next to the ribs with the exposed periosteum, a layer of vascularized connective tissue that surrounds the bones. Bone tissue was then allowed to grow from the periosteum into the bioreactor over a period of nine weeks. After that time, the researchers removed the spacers from the lower jaws and implanted tissue grown in the bioreactor in their place. The researchers found that the two materials grown in the bioreactors that were initially filled with ceramics or crushed bone were sufficient for implantation; However, tissue grown from crushed bone had mechanical properties more similar to natural bone, so they used them in the final implantation procedure.
Twelve weeks after implanting the bioreactor-grown tissues into the jaw, the researchers observed new bone bonding to natural bone and soft tissue growing to cover the wound site. The results demonstrated that viable bone tissue that could replace grafts taken from the leg, the current clinical procedure, could be manufactured from bone materials grown with 3D-printed bioreactors.
The research was funded in part by NIBIB (EB023833), the National Institute of Dental and Craniofacial Research (DE027586), the National Institute of Arthritis and Musculoskeletal and Skin Diseases (AR071258 and AR067606), all parts of the National Institutes of Health, as well as a grant from the Armed Forces Institute for Regenerative Medicine co-sponsored by the NIH. (W81XWH-14-2-0004). Additional support for the research came from the Osteo Science Foundation, the Barrow Scholars Program, and the Robert and Janice McNair Foundation.
Biomaterial-assisted mandibular reconstruction using in vivo bioreactors. Tatara AM, Koons GL, Watson E, Piepergerdes TC, Shah SR, Smith BT, Shum J, Melville JC, Hanna IA, Demian N, Ho T, Ratcliffe A, van den Beucken JJJP, Jansen JA, Wong ME, Mikos AG. Proc Natl Acad Sci US A. March 18, 2019.